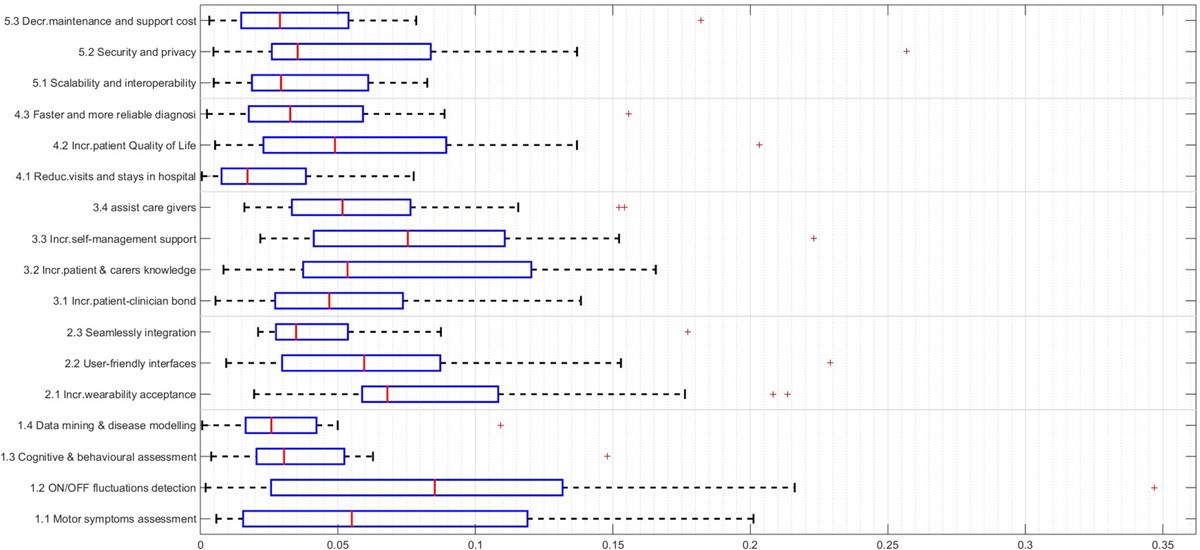
The limited availability of information on large-scale performance and economic impact might account for some of these perceptions. Yet, there is a widespread perception that telemedicine applications are not as widely used as expected. This would result in improved level of care measured through target indicators like number and quality of visits, access to emergency departments and ambulance services, number of hospitalizations, hospital readmissions, and length of hospital stay, number of referrals, duration of consultations, number of laboratory tests, and avoided transfers/evacuations. Telemedicine could contribute to optimize the use of health services in PD management by delivering care services in daily living environments and strengthening the connection between patients and care providers. Progression of the disease is strongly correlated with higher costs - for both patients and healthcare institutions - and substantial savings can be achieved by slowing down this progression. As other chronic diseases, PD is a prolonged condition that does not improve with time and cannot be cured completely. Parkinson's disease (PD) is a neurodegenerative disorder affecting more than 1% of people older than 60 years (and with an increased prevalence in older subjects). This framework can be used to support the decision-making process for the adoption of new technologies in PD. Moreover, the AHP effectively supported the user need elicitation as well as the assignment of different weights and priorities to each need and, consequently, it helped to define a framework for the assessment of telehealth systems for PD management and monitoring. Conclusionsįirst of all, the AHP contributed to the elaboration of a unified hierarchy, integrating the needs of a variety of stakeholders, promoting the discussion and the agreement into a common framework of evaluation. These results have been used to evaluate the PERFORM system and to identify future areas of improvement. No significant differences were found between the clinician and technical groups. On/Off fluctuations detection, Increase wearability acceptance, and Increase self-management support have been identified as the most relevant user needs. A total of 16 experts, 6 of them with a clinical background and the remaining 10 with a technical background, were asked to rank these needs and categories. MethodsĪnalytic Hierarchy Process (AHP) was used to design a hierarchy of 17 needs, grouped into 5 categories. This work aims to 1) identify the most relevant user needs of a new medical technology for managing and monitoring Parkinson's Disease (PD) patients and to 2) use these user needs for a preliminary assessment of a specific system called PERFORM, as a case study. This lack of information may limit the future development and deployment in the clinical practice. This task is even more delicate when the assessment is carried out in early stage of development processes, when the maturity of the technology prevents conducting a large scale trials to evaluate the cost effectiveness through classic health economics methods. The assessment of a new health technology is a multidisciplinary and multidimensional process, which requires a complex analysis and the convergence of different stakeholders into a common decision.
